The Diagnosis
Sitting on the table in the doctor’s office, the words came as a shock:
“You need Partial Knee Replacement surgery.”
I thought to myself, you have to be kidding. Me? I’ve never had any kind of surgery, never had any broken bones, I was a dedicated and consistent runner and, most importantly, a very active SCUBA diver. How could this be?
This journey started several months earlier when I noticed some stiffness and discomfort in my left knee during a routine early morning run in my neighborhood. I immediately stopped, and avoided running for a few days. When I again tried to run, I had the same discomfort and I noticed that my knee was a little swollen.
Convinced that I just needed to rest the knee, I stopped running for several weeks but then I competed in a local 5K that I had signed up for earlier. That was not smart; my knee was in much more distress after that.
This was problematic – a dive trip to Malta was on the horizon in a few weeks. I needed to get me knee healed…from whatever I had done to it!
After more rest, I did manage to get through the dive trip without incident, and promptly went to an orthopedic knee doctor immediately upon my return. MRIs, X-Rays and physical examinations confirmed that there was no meniscus tear or bone damage. There was, however, some cartilage damage that likely was causing the pain and discomfort. The doctor drained the knee of fluid, reducing the swelling, and gave me a cortisone shot.

Post-surgical X-Ray show the implants (indicated by bright white objects)
As uncomfortable as all of that was, within a day or two my knee felt better than it had in years! I stubbornly entered another 5K race and completed the event without incident…or so I thought. By the time I got home from the race, the swelling had returned and I could put no weight on my leg whatsoever. I learned this by falling to the ground when I tried to get out of my car!
This led to a follow-up with the knee doctor and the prognosis he rendered: Partial Knee Replacement Surgery.
What is Partial Knee Replacement Surgery?
Partial knee replacement is a surgical option for patients who have developed arthritis in only one portion of the knee. This is called unicompartmental osteoarthritis of the knee. It is a condition in which degenerative arthritis affects only one part of the knee joint, while the other regions (or “compartments”) of the knee remain healthy or not significantly damaged.
This was my diagnosis.

A model of the human knee.
In partial knee replacement surgery, the bone surfaces of only one compartment of the knee joint are removed and replaced with implants. In total knee replacement surgeries, all the compartments of the knee are replaced. During the procedure, damaged cartilage and bone is removed from the diseased area only, leaving the rest intact.
Although partial knee replacements are less common than full knee replacement procedures, improvements in surgical techniques have made partial knee replacement an increasingly attractive option for a growing number of patients. Recent data indicates that between 10% to 25% of all patients with osteoarthritis of the knee needing replacement surgery may be eligible for this procedure.
All of this sounded good, but my over-arching concerns had to do with returning to the activities I love…notably, running and SCUBA Diving.
“Well, you’re running days are over,” said the doctor. I held my breath for the second part of the sentence: “But SCUBA Diving, you should be good to go after some physical therapy. In fact, SCUBA Diving is one of the recommended activities for patients with this procedure.”
A big sigh of relief!
The Surgery: what to expect
The surgery was scheduled for 10 weeks later. In those ten weeks, I worked with my health insurance company to approve the procedure, prepared my house for the recovery period, purchased a cane and a walker, and completed pre-surgical testing.
The surgery was done with a combination of general anesthesia and a nerve blocker in the spine. Like all general anesthesia, this is the best sleep you’ll ever have! I did get a glimpse of the robotic machines that were used in the surgery just before blacking out!
My procedure was a Mako Robotic-Arm Assisted Partial Knee Replacement.
Mako Robotic-Arm Assisted Technology is used to create a personalized surgical plan based on your unique anatomy. Prior to the surgery, a CT scan of the diseased knee joint is taken and uploaded into the Mako System software. A 3D model of the knee is then created. This 3D model is used to plan the surgery and to assist your surgeon during the procedure.

MAKO Robotic assisted surgery can result in better outcomes
In the operating room, the surgeon follows your personalized plan while preparing the bone for the implant. The surgeon guides the robotic-arm and the Mako System helps the surgeon stay within the planned boundaries that were defined when the personalized plan was created prior to the operation.
In my case, the bone was shaved, implant covers attached to the bones and the meniscus removed and replaced with another substance to help cushion the joint.
I was glad I wouldn’t be awake to see this!
I was told the procedure took a couple of hours. When I woke up in recovery, my legs were still “paralyzed” and it was a strange sensation to not be able to move them. But within a few hours, I was up and walking and, with the assistance of a physical therapist, walking up a flight of stairs albeit it very carefully. I was released to go home that same day.
Initially, there was no pain, just a feeling of tightness. A large dressing had been applied and the wound was sealed with surgical glue.
Now the recovery would begin.
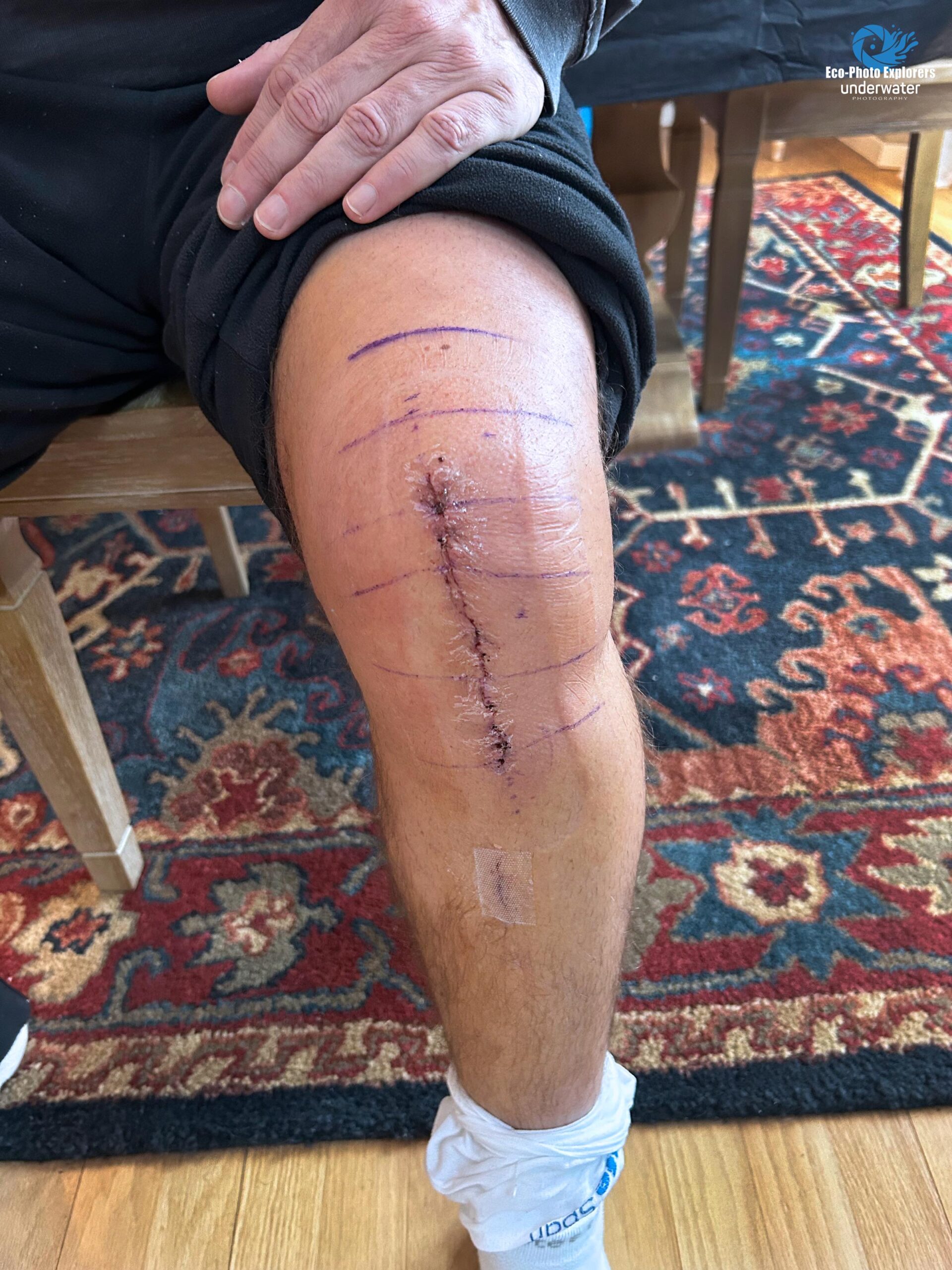
Shortly after the surgery with the surgeon’s ink markers still on the skin
Post-surgery: recovery and rehab
For the first few weeks after the surgery, the regimen is to rest the leg, begin in-home physical therapy immediately, apply ice every two hours, and adhere to the schedule for the prescribed cocktail of medications. In this case, the medications included several varieties of pain relievers, aspirin to prevent clots, medicines for gastric protection and , to prevent constipation, along with antibiotics to prevent infection.
In my case, I developed an allergic reaction to the surgical glue (Derma Glue) which resulted in severe itchiness on both legs. An over-the-counter antihistamine was prescribed to help alleviate this.
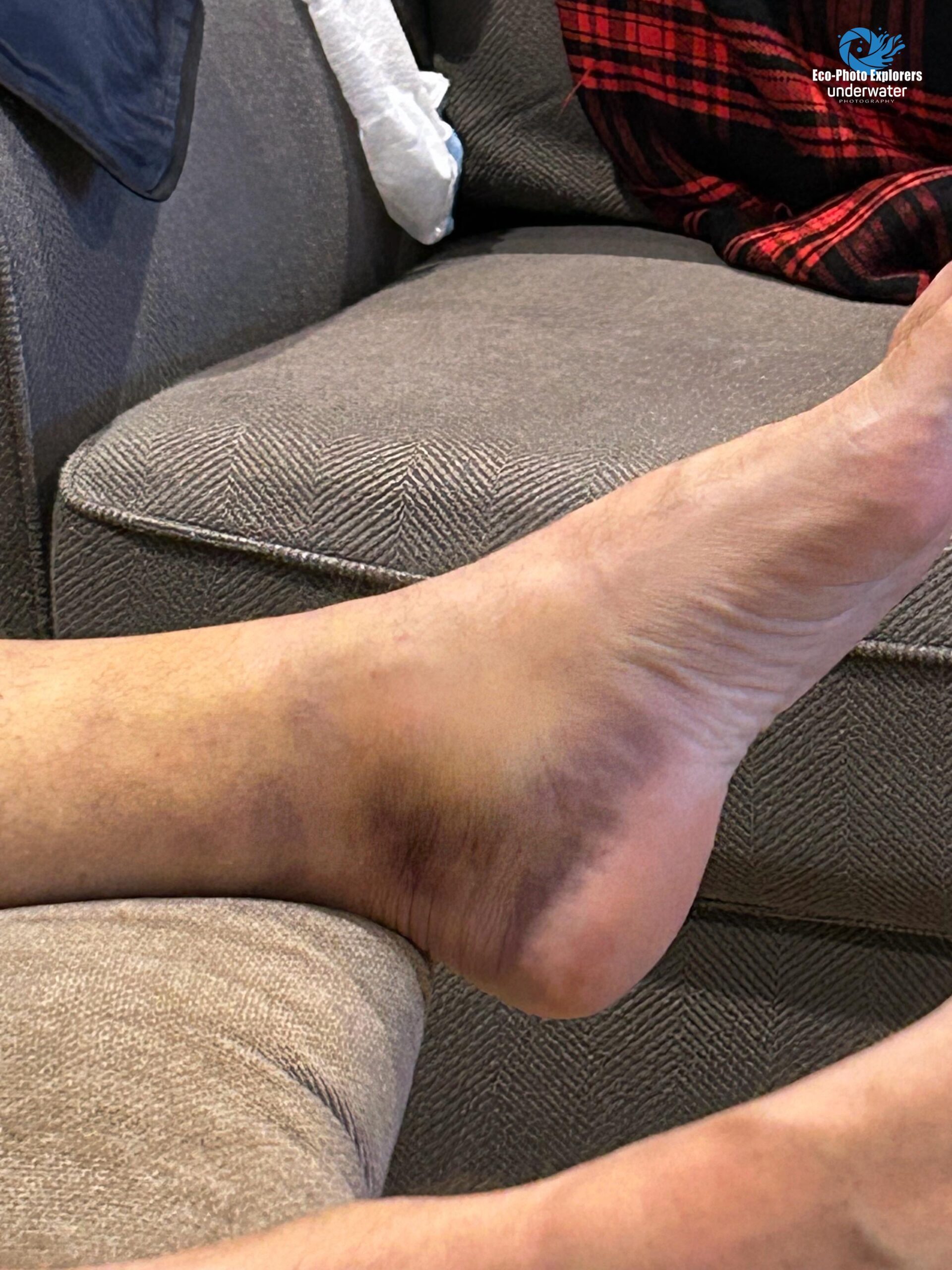
A few days after the knee surgery bruises and swelling in the ankle and foot
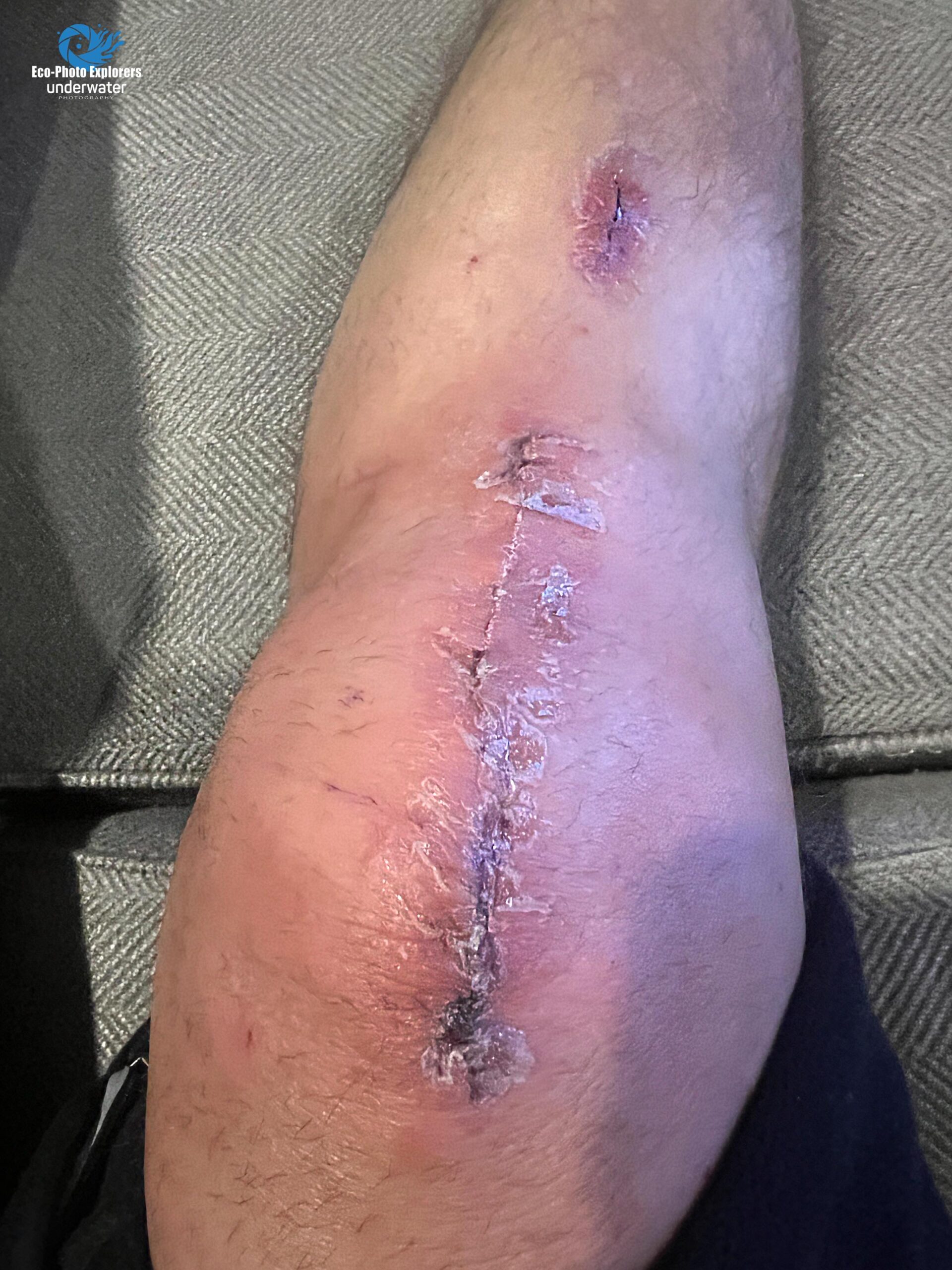
The scars from the incisions as they appeared after the packing was removed
Words & Photos by Michael Salvarezza and Christopher P. Weaver
One of the most important aspects of recovery is the physical therapy. The exercises that are prescribed help to strengthen the knee, promote healing and most importantly improve the range of flexibility and motion. They are uncomfortable, especially at first, but they are absolutely effective and necessary. For several weeks, I adhered to a strict schedule of exercises every two hours followed by 20 minutes of ice.
Despite all of this, I was walking fairly normally only a few days after the surgery. I used the walker once – to get from the car into the house on the day of the surgery. I used the cane for one day. After that, I walked on my own.
The bandages and packing were removed after 10 days. The incision looked a little ugly but I was glad to have it exposed to the air finally. After 3 weeks, I did a follow-up with the doctor who examined the knee, the incision and the overall progress. He cleared me to resume driving, which was a good step forward for me.
At this point, physical therapy out of the house began, with a twice-a-week regimen of more intense exercise and a battery of in-home exercises to be done every day.
After three weeks, I was also able to attend the Boston Sea Rovers Underwater Clinic and the Beneath the Sea dive shows where I presented seminars and introduced other speakers. Although my knee would get fatigued and I frequently had to rest, I was thrilled that the surgery did not prevent me from attending these shows.
And after 5 weeks, I was on a plane to California for a business conference. I was surprised that even though I now had titanium implants in the knee, I did not set off the TSA metal detectors! While not fully returned to normal, I did feel good about the pace of progress in my recovery.
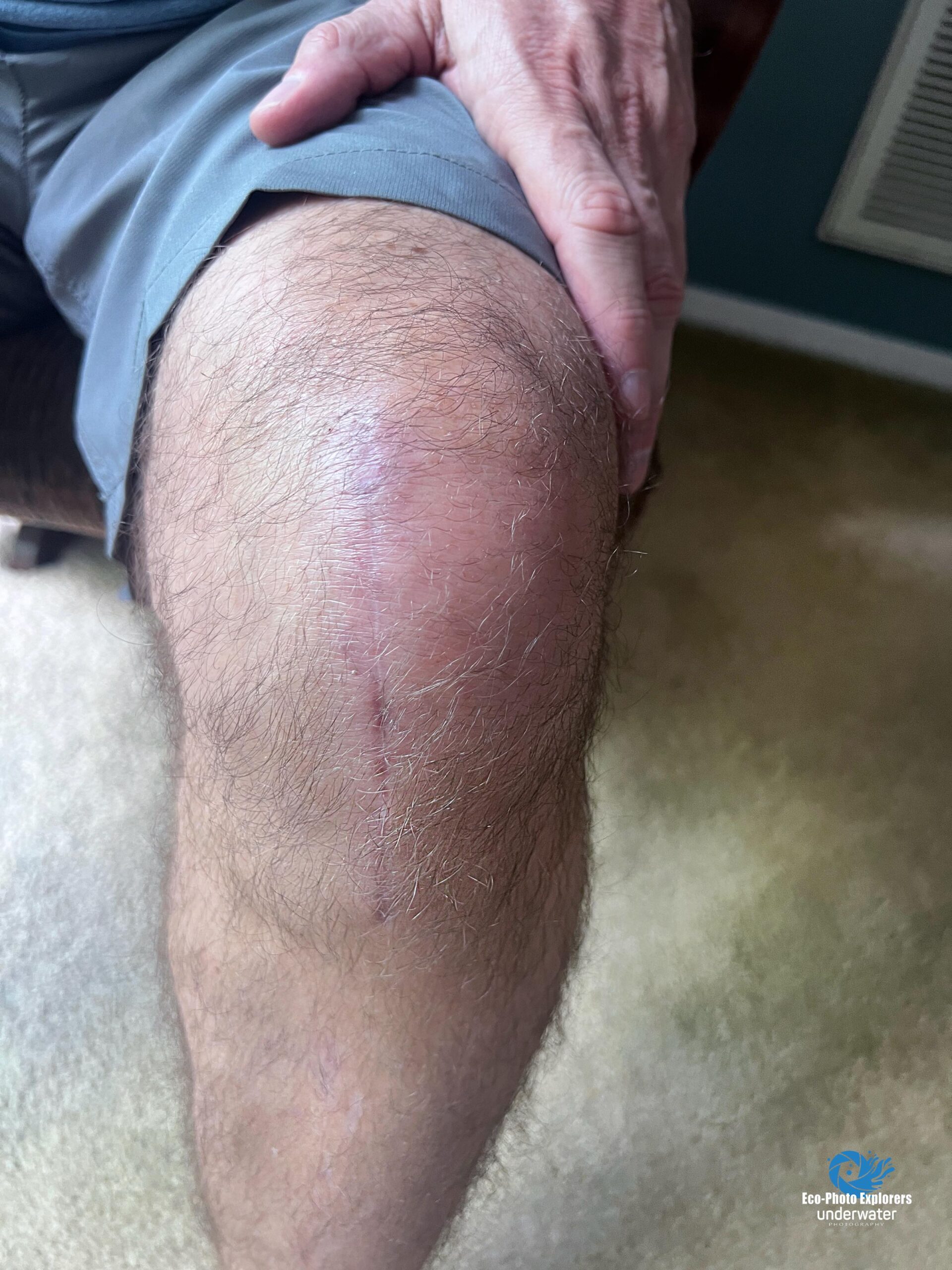
90 days after surgery the scars have healed nicely but some swelling remains
The Return to Diving
My doctor was hesitant to approve diving activities until the incision fully healed. It took 90 days until I was finally cleared to get back in the water. As soon as I got that good news, I arranged with a local dive shop to make use of their training pool to do a test. I wanted to not only immerse the knee, but to test my strength for all the normal diving activities you could routinely expect: carrying the equipment, suiting up, standing up from a bench with full gear on, giant stride entries and, most important, mobility, strength and flexibility under the water. I did not want to jump off a boat and discover I had problems so the pool test became paramount in my opinion.
The result was a perfect test. I felt as if the knee was pain free, strong enough and flexible enough under water to be safe for diving. Being under water on SCUBA, even though it was just in a pool, felt exhilarating after this medical journey.

Checking the dive gear before the pool session

The return to the water!

Even in a pool, being under water was exhilarating
There are still lingering effects. My knee is still somewhat swollen. The doctor says this might take 6 months to fully resolve. There is a portion of my leg near the knee that is still numb. The doctor says this is a result of the severing of nerves during the surgery. While he is hopeful this will resolve over time, he also says this may never fully return to normal. Kneeling directly on my knee is problematic, mostly because it feels strange, almost as if I have packing material on the knee. But none of these issues are affecting my ability to walk, go up and down stairs, drive my car or, most importantly, SCUBA dive.
And so now, after partial knee replacement surgery, and 90 days of rehabbing, there is only one thing left to do: find the next dive destination and book the trip!
Postscript
After nearly a year and a half since the surgical procedure, I am happy to report that the knee is functioning well. I experience no pain and have no difficulty walking whatsoever. More to the point of this article, though, the great news is that diving is completely unaffected by the surgery: I have completed over 50 dives in various conditions ranging from shallow tropical reefs to deep shipwrecks and the knee feels as strong as ever.

Exploring a shipwreck in the Sea of Cortez shortly after recovering from the surgery
Words & Photos by Michael Salvarezza and Christopher P. Weaver
